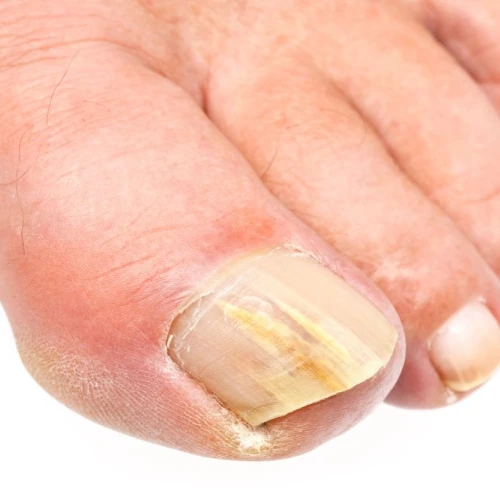
What are the symptoms of a fungal nail infection?1, 2
Fungal nail infections are often caused by microscopic fungi. The first symptom is the impact on the periungual tissue (area around the nail). This area becomes red, swollen and painful, sometimes accompanied by a discharge of clear liquid. A yellowish patch will appear on the edge of the nail which will gradually spread. The nail then thickens. The fungal infection will gradually spread and reach the nail matrix which becomes discoloured and whitish in colour. The nail will partially detach. Fungal nail infections are diagnosed after lab testing a sample of the fungus.
What causes fungal nail infections?2
Onychomycosis is caused by the presence of a microscopic fungus. There are three types:
- Anthropophilic dermatophytes (tricophyton rubrum in 80% of cases or mentagrophytes in 20% of cases).
- Candida genus yeasts (candida albicans in 70% of cases or candida parapsilosis).
- Moulds.
These fungi colonise the nail and proliferate, thus weakening the nail plate. The nail will then become discoloured, misshapen and fall off.
How do you catch a fungal nail infection?2
Dermatophytes are the most common cause of a fungal nail infection and are generally transmitted via self-spreading. This means that the trigger for a fungal infection is already present on an area of skin close to the nail. Fungal nail infections are often preceded by fungus affecting the skin between the toes (the famous “athlete's foot”).
Dermatophytes infection can also be spread by a person who has shed flakes of infected skin over the ground. Walking barefoot in public places (e.g. swimming pools, saunas, changing rooms, sports halls) is a risk factor for infection.
Candida genus yeasts proliferate under nails weakened by prolonged and repeated contact with water. They are much more common in fingernails.
As far as moulds are concerned, it is much easier to catch them when walking barefoot.
How do you treat a fungal nail infection?2
Treating a nail fungal infection is often lengthy and burdensome. Several treatment options are possible, which can be combined.
Topical treatments
Topical treatments are prescribed as a first-line option when the fungal infection only affects part of the nail, and the matrix is unaffected. Topical treatment for a fungal nail infection requires:
- Application of a urea-based cream to strop the nail. The cream must be applied every day under an occlusive dressing (i.e. air- and water-tight) which is kept on 24 hours a day and replaced after each shower. The diseased part of the nail is softened and can be easily removed by scraping or cutting it off. Cream should be applied for 2-4 weeks.
- The daily application of an antifungal nail polish for 3-6 months. This step generally follows the urea-cream stripping stage. The varnish should be used daily until a healthy nail has fully grown back (this generally takes around 3-6 months).
- Disinfection of footwear using an antifungal powder.
Oral treatments
Oral medication is required when:
- Topical treatments have not cured the fungal infection;
- Several nails are affected;
- The nail matrix is affected.
They are usually combined with a topical treatment.
Lasers
Some dermatologists offer Long Pulsed Nd:YAG lasers which have been shown to be effective in treating fungal nail infections. These lasers destroy heat-sensitive fungi. Four sessions spaced one week apart are generally sufficient to sterilise the affected nail. Laser treatments are generally combined with topical treatments.
Surgery
Fungal nail infections caused by moulds may require the surgical removal of the nail. Surgery is more effective than topical and oral treatments.
What are the risk factors?2
Some factors are known to increase the risk of fungal nail infections:
- Age: after the age of 60, 1 in 3 people suffer from nail fungal infections, which is linked to slower nail growth and blood circulation problems.
- Some conditions such as diabetes and Cushing's syndrome.
- Some skin conditions that affect and weaken the nails (psoriasis, lichen).
- Immuno-suppression due to HIV, immunosuppressants, chemotherapy, etc.
- Blood circulation disorders.
- Repeated trauma to the nails (knocks, bruises, cuts, etc.).
- Moisture caused by excessive perspiration, wearing closed shoes all the time, contact with water or food (cleaning ladies, catering professionals, etc.).
- Walking barefoot in public areas potentially infected with fungi (swimming pools, saunas, sports halls, etc.).
How do you reduce the risk of fungal nail infections?2
You can reduce the risk of contracting a fungal nail infection by following a few simple steps:
- Avoid contact with water and/or caustic products by wearing cotton and rubber gloves;
- Wear shoes fitted to the shape of your feet and toes (i.e. not too tight);
- Do not wear closed-toe shoes for prolonged periods and let your feet breathe as much as possible;
- Do not walk barefoot in public areas to avoid coming into contact with surfaces that may have been infected with fungi.